Semaglutide May Reverse Damage Caused by Osteoarthritis, Study Suggests
Medical researchers have discovered that semaglutide may reverse the debilitating tissue damage caused by osteoarthritis, the world’s most common form of arthritis.
The drug behind Ozempic and Wegovy is best known for treating type 2 diabetes and helping people lose weight. But the new study found semaglutide appears to protect joints in mice through a mechanism that’s not about easing pressure through weight loss.
Instead, the drug reprograms the metabolism of cells that synthesize and maintain healthy cartilage, allowing them to generate more energy.
“This work not only highlights the potential off-target effect of semaglutide as an effective drug to treat metabolic osteoarthritis,” the team from China and the US writes in their published paper, “but also reveals a weight loss-independent repair mechanism.”
In addition to mouse experiments, the researchers also conducted a randomized human trial to assess the effects of semaglutide on pain, mobility, and tissue degradation in individuals with osteoarthritis and obesity.
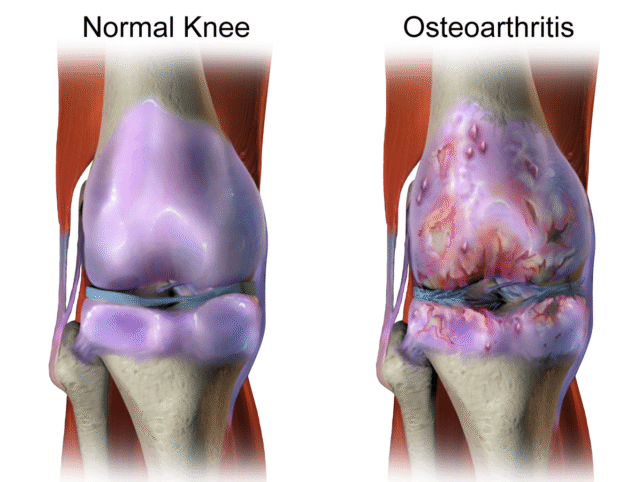
Obesity, metabolic disorders such as diabetes, and inflammation are major contributors to osteoarthritis progression. These conditions can affect just about every tissue in the body, including bone, cartilage, and synovium (the lubricating membrane lining the inner surfaces of joints).
Semaglutide-based drugs like Ozempic and its kin work by mimicking glucagon-like peptide 1 (GLP-1), a natural hormone that stimulates insulin release to manage blood sugar levels. This hormone also tells the brain that mealtime has concluded, facilitating an appetite-suppressing effect.
Therefore, it seems obvious that weight loss eases osteoarthritis by reducing load-bearing forces on the joints. But this isn’t always the case. Existing osteoarthritis therapies are generally palliative. So while they may alleviate the symptoms, they don’t address the underlying cause.
But semaglutide appears to affect joint health at a fundamental level. In mice and humans with obesity and osteoarthritis, treatment with semaglutide reduced pain and decreased cartilage degeneration. Mice also had fewer bone spurs and less severe lesions in their joint membranes.
When the researchers compared cartilage from treated and untreated mice, they detected changes in the expression of nearly 8,300 proteins.
They included a crucial control: a “pair-feeding” group that ate the same amount as the semaglutide-treated mice. Even with comparable weight changes, the pair-feeding group did not receive the same cartilage protection, suggesting a weight-loss-independent effect on the joint itself.
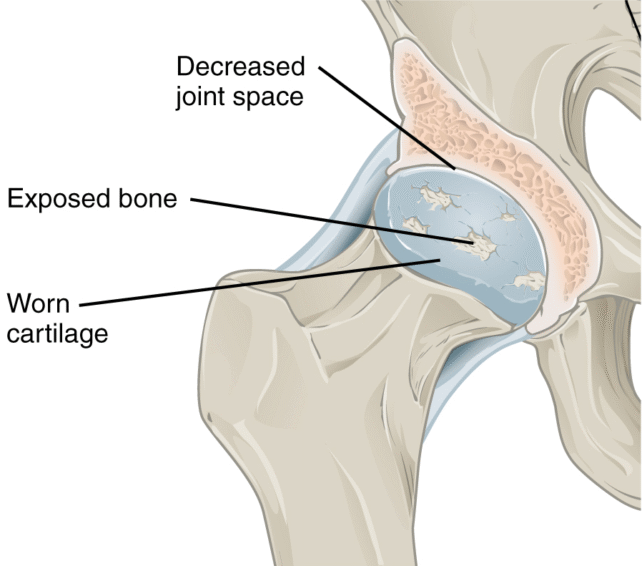
Yet it seems the most important biological pathway altered by semaglutide is the “GLP-1R-AMPK-PFKFB3 axis,” a cascade of compounds that affects how various cells produce energy.
By initiating this cascade of enzymes, semaglutide alters the metabolic processes used by chondrocytes (cells found in healthy cartilage), making them more efficient and allowing them to survive.
As the researchers revealed, a process called glycolysis generated most of the energy for chondrocytes in osteoarthritis-affected mice.
Glycolysis doesn’t require oxygen, so it supplies energy quickly during stressful, high-intensity exercise, like the morning sprint to catch the garbage truck. Yet, due to the lack of oxygen, glycolysis produces only two net ATP (energy-providing) molecules per glucose molecule.
But after semaglutide treatments, a process called oxidative phosphorylation (OXPHOS) became the preferred metabolic pathway for chondrocytes. Unlike glycolysis, OXPHOS uses oxygen and produces much more ATP, up to 36 molecules per glucose molecule.
To see if any of this might translate to humans, the researchers recruited 20 individuals, aged 50-75, with both obesity and osteoarthritis, and randomly divided them into two groups. One group received sodium hyaluronate (HA), a joint-lubricating, especially effective form of hyaluronic acid. The other group received both HA and semaglutide.
At the end of the 24-week treatment period, the HA+semaglutide group experienced lower osteoarthritis pain scores and substantial improvements in knee function. MRI analysis also revealed thicker cartilage and recent cartilage growth in the inner joint areas that bear weight and absorb shock from daily movements.
The findings from this study may impact global healthcare outcomes. Osteoarthritis affects around 600 million people globally and is forecast to afflict one billion people by 2050. It’s also increasing among younger, active populations, leading to decades of pain and disability.
The work adds to growing evidence that GLP-1 drugs may have benefits beyond weight loss, and it sharpens the search for new osteoarthritis treatments that target metabolism inside the joint.
Related: Will Exercise Help Your Osteoarthritis? A New Review Has Surprising Findings
It is also worth keeping expectations in check. Mouse studies do not always translate to long-term human outcomes, and semaglutide use has its own not-so-rosy side effects and concerns.
“The protective effects of semaglutide on the human knee joint should be interpreted with caution and require further validation by clinical trials,” the researchers conclude.
This research was published in Cell Metabolism.
What did you think of this news? Leave a comment below and/or share it on your social media. This way, we can inform more people about the hottest things in technology, science, innovation, and gaming!
This news was originally published in:
Original source